Paying the Price for Harm Reduction Budget Cuts
Hungarian needle and syringe exchange programs are facing financial problems because the government is not budgeting enough money for harm reduction services. Experts predict this could result in dramatically increased prevalence of HIV/AIDS among injection drug users- such as that currently being experienced in Romania.
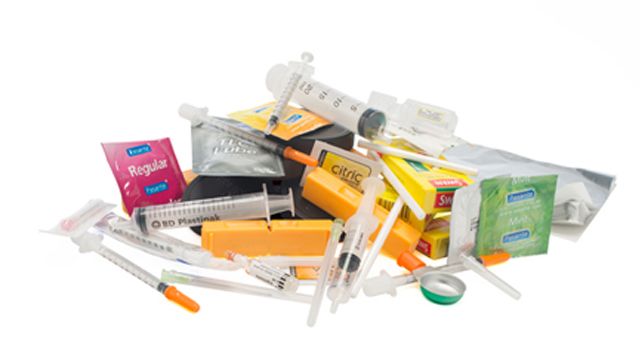
Hungarian needle and syringe exchange programs are facing financial problems because the government is not budgeting enough money for harm reduction services. Experts predict this could result in dramatically increased prevalence of HIV/AIDS among injection drug users- such as that currently being experienced in Romania.
The “Magdolna negyed” is an area in the 8th district of Budapest that is home to many low- income Hungarians and members of marginalized groups like the Roma. A mixed neighborhood where many working people and families live and play, it has areas of problematic intravenous drug use. When Kék Pont (Blue Point) opened its government and private funded needle & syringe program (NSP) there in 2006, demand was high. More than 10.000 needles were distributed to about 300 clients during the first six months (compared to 1000 needles for 100 clients when Kék Pont operated in a different district). In 2012 Kék Pont distributed 122.892 syringes to between 1200-1400 clients who used the NSP at least once during the year. Now the money has run out though, Kék Pont is running out of needles and condoms. They can only distribute five needles per person per day. Given that new psychoactive substances are injected up to 20 times a day, this is a catastrophe, and underlines the increasing need regular distributions of sufficient clean needles.
The new psychoactive substances and problems that come with it
The new psychoactive substances, most of which are not legally regulated, have become popular within the last three to four years. According to the data of the Hungarian Reitox National Focal Point, monitoring drug use and drug addiction in Hungary, heroin use has declined and people who inject drugs (PWIDs) switched to “other” substances (mostly new psychoactive substances). In 2010, 47% of PWIDs attending NSPs injected heroin. By 2012, that number had dropped to 17%. In 2010, 8% of PWIDs attending NSPs injected “other types of substances,” and in 2012 approximately 43% did so (provisional data, NFP). This is known as “the balloon effect.” Meanwhile though, amphetamine use remained quite stable.
One problem with the new psychoactive substances is that, since the street names of the drugs don’t always correspond to their actual content, PWUD don’t always know what’s in the fix. Worse still, they need to inject the new drugs more frequently: 10, 15, sometimes up to 20 times a day as opposed to 3, 5 or 7 times a day for heroin.
Roland Gyékiss, social worker at the NSP of Kék Pont remembers that in 2011 Kék Pont distributed a record number of more than 220,000 needles.
Because the new psychoactive drugs have to be injected more frequently, the side effects of addiction are visible earlier compared to other drugs. However, there is still not enough information. By the time professionals have adequate information (about their psychological effects for example) the drugs have usually already disappeared from the market.
Government funding for NGOs and their current financial situation Hungarian NGOs can bid for three-year state grants (6 million HUF a year) for harm reduction services (“low-threshold programs”). Because a new funding period began in 2012, the government could select a different set of grantee organizations.
Hungarian NGOs can bid for three-year state grants (6 million HUF a year) for harm reduction services (“low-threshold programs”). Because a new funding period began in 2012, the government could select a different set of grantee organizations.
Generally speaking, the programs have achieved better geographical coverage. Before 2012, there were only 24 NSPs. Now there are twenty-nine, in five more Hungarian cities (provisional data, NFP). In order to adequately meet current need though, Budapest and Miskolc services need more funding. For instance, a mobile NSP in Miskolc, a city in Northeast-Hungary with serious intravenous drug use (IDU) and Hepatitis C problems had to close its doors last year. In Budapest, a Kék Pont outreach program had to close and ArtEra, the third biggest NSP in Budapest, was shut down for six months. When several NGOs collaborated and were given a “second chance” to apply for state financial support, Kék Pont and ArtEra were able to re-open in June 2012.
The HCLU has led the campaign to protect harm reduction services. We have published several blogs, articles in the most popular online and printed journals, and attended television and radio shows to raise public awareness. A debate between the head of the Youth Department of the Ministry of Human Resources (EMMI), who is the government official responsible for drug affairs, and the drug policy program director of the HCLU was televised and broadcasted on one of the most popular television channels, ATV. Additionally, we have prepared two short videos on NSPs: one on the general situation of harm reduction programs and the risk of an HIV epidemic among PWIDs in Budapest, the second on a special NSP service for women who use drugs (Change for Chicks). Both videos were widely distributed and published by the largest Hungarian online media (Index).
As a result, HCLU was contacted by a private foundation in fall 2012, which donated 100.000 needles and syringes to the three biggest NSPs in Budapest. The video on the NSP service for women attracted the attention of a private donor who gave 3 million HUF to maintain this service. Moreover, the government was forced to provide 6 million HUF in emergency aid that distributed among the biggest Hungarian NSPs in need. In May this year the government provided another 7 million HUF to NSP programs.
However, it is not clear what qualifies some NGOs rather than others to receive government funding. Levente Móró, editor of the homepage of the Hungarian psychedelic drug use community, thinks the NGO money is not distributed professionally. “There are fears that if anyone criticizes the ministries, they cut off their funds. It’s a power game.” Móró believes that few people in Hungary have in-depth expertise in drug issues, since those that do are mostly not in government ministries but in universities and NGOs. Móró emphasizes the importance of NGOs working in the drug field, since they are more aware of the actual drug situation and hence more likely to reach drug users. Because they have more expertise and can respond more rapidly, the money they receive – if they receive it – should be provided much faster.
“I think it is essential to maintain the current programs and those that have been up and running for a while. It is really sad that many people had to leave their drug profession because NGOs couldn’t pay their staff and had to let them go. The funding cuts have largely weakened the drug NGO scene.” Another thing that has changed in the new funding period is that NGOs can no longer apply for “extra” grants. Since this special funding stream no longer exists, NGOs have no emergency money for unforeseen needs and injection equipment. Besides, the financial crisis means there is not as much money in the system. The 2012 provisional data of the National Focal Point revealed that 35% fewer syringes were distributed last year, and fewer used syringes were collected. The needle exchange services became less accessible, although the number of clients remained constant. Although Kék Pont receives 6 million HUF funding for running its NSP, in 2011 they spent approximately 5 million HUF on supplies. Operating costs were over 10 million HUF.
Another thing that has changed in the new funding period is that NGOs can no longer apply for “extra” grants. Since this special funding stream no longer exists, NGOs have no emergency money for unforeseen needs and injection equipment. Besides, the financial crisis means there is not as much money in the system. The 2012 provisional data of the National Focal Point revealed that 35% fewer syringes were distributed last year, and fewer used syringes were collected. The needle exchange services became less accessible, although the number of clients remained constant. Although Kék Pont receives 6 million HUF funding for running its NSP, in 2011 they spent approximately 5 million HUF on supplies. Operating costs were over 10 million HUF.
The Baptist Aid “Utcafront”, a shelter for homeless drug users, runs two storefront NSPs as well as the only mobile NSP in Hungary. Although the 6 million HUF they receive from the government for running their mobile NSP doesn’t cover the petrol for the van or staff salaries, it is better than nothing. But the two storefront NSPs are now in danger of closing since as of 2012 they no longer receive sufficient government funding for all three programs.
Dr. József Csorba is a physician at the opiate substitution center of the “Nyírő Gyula Hospital” in Budapest, which is one out of nine in the whole of Hungary. (Three are in Budapest, the other ones in Miskolc, Szeged, Pécs, Veszprém, Gyula and Eger but the Northwest and Northeast regions have no OST coverage.) Dr. Csorba’s drug ambulance currently supplies methadone and buprenorphine (Suboxone) to 456 patients. Although he doesn’t believe their funding has changed, much he did say that the former government offered more grants than the current one. In the last two years these grants have become “minimal”, and are now used for treatment and prevention programs. Furthermore, in his opinion society’s general attitude toward drug users has changed. Drug users are now expected to be abstinent and go to rehab rather than use harm reduction services.
The limited budget of the drug ambulance affects how medications are dispensed. Although the recommended therapeutic dose of buprenorphine is 12-14 mg, patients can only get 8mg per day. Buprenorphine is preferred to methadone, which must be injected and therefore always carries the risk of overdose and addiction. The problem is that it is 10 times more expensive than methadone. Because methadone supplies are limited, names of people in need (except for pregnant women and those who are HIV positive) are put on a waiting list and have to wait for that medication for 2-3 months. In order to provide adequate psychotherapy, psychosocial interventions, and hire qualified staff. the program needs approximately 30-35 million HUF more per year. At the moment, only one social worker and two psychologists work at the center.
Dr. Zsolt Demetrovics, a psychologist at ELTE University, doubts that the government’s abstinence-only approach to the drug problem will succeed. However, he believes the reason is a lack of money in the system, rather than a lack of political will to support harm reduction.
“None of the former governments did much on [the drug issue]. But before 2010 there was more money in the system. It was not a very different approach, I mean although it was not very supportive there was still more money for the NGOs and harm reduction programs. That’s the difference now. Although the current government is more critical of harm reduction in theory, that’s not the problem. I mean previous governments have also criticized harm reduction but still provided financial support.”
According to Peter Portörő, drug coordinator for the former government, his administration had recognized that problematic users were “sick” and emphasized treatment rather than punishment. The new criminal code gives people who use drugs only one chance in two years of accessing treatment. If they are caught again they can be sentenced to jail.
Hepatitis C prevalence
The National Center for Epidemiology data of 2011 revealed that Hungary had a 24% Hepatitis C rate among PWIDs compared to a 34% rate in Budapest. The same study showed that the Hepatitis C prevalence was usually significantly higher among women (esp. those 25 and older) than men. Those who injected amphetamine, cocaine and new psychoactive drugs had a 30% Hepatitis C prevalence rate compared to 18% for opioid injectors. This reverses previous rates, which were 30% for opioid injectors, and 16% for non-opioid injectors. Moreover, the fact that heroin has disappeared from police drug seizures indicated that PWIDs probably changed from heroin use to the use of new psychoactive substances.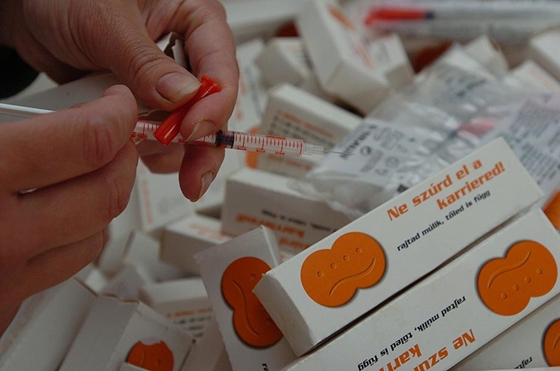 In a joint project with the National Center for Epidemiology, Kék Pont tested PWIDs in Budapest for Hepatitis C and HIV in 2011. Approximately 75% tested positive for Hepatitis C. Budget cuts have prevented further screenings of this sample size. There is a need to repeat Hepatitis C and HIV national prevalence study among PWIDs in order to gather data on 2012 developments, following the more frequently injection of new psychoactive substances and restricted availability of syringes.
In a joint project with the National Center for Epidemiology, Kék Pont tested PWIDs in Budapest for Hepatitis C and HIV in 2011. Approximately 75% tested positive for Hepatitis C. Budget cuts have prevented further screenings of this sample size. There is a need to repeat Hepatitis C and HIV national prevalence study among PWIDs in order to gather data on 2012 developments, following the more frequently injection of new psychoactive substances and restricted availability of syringes.
The new psychoactive substances pose challenges for drug treatment. Because so little is known about their pharmacology, and users often don’t know what they have been taking, treatment centers have few tools with which to respond. That issue, coupled with NGO budget cuts, creates the public health nightmare of more drug users being infected with more blood borne diseases.
While Hepatitis C prevalence is already extremely high among PWIDs in certain areas in Budapest, fortunately HIV is not yet an issue in Hungarian IDU population. But unless the government increases funding for harm reduction and recognizing its importance, Hungary will face an HIV epidemic much like the one in Romania.
This article was written by Katharina Grimm, the intern of HCLU from April to September 2013. It is based on interviews that were made with several experts working in the drug field. Many thanks go out to everyone who shared their knowledge, information and precious time with me, in order to make this article happen. Thanks to Katherine Pettus for proof-reading, copy-editing, and teaching me just a few of the many subtleties of the English language.







